
TRT Fundamentals:
Understanding Testosterone Therapy
A comprehensive, plain-language guide to testosterone replacement therapy. Whether you are researching for yourself or a loved one, this page covers the science, the symptoms, the treatment options, and what you can realistically expect.
What Is Testosterone?
Testosterone is the primary male sex hormone, though women also produce it in smaller amounts. It belongs to a class of hormones called androgens. In men, testosterone is mainly produced in the testes, with small amounts coming from the adrenal glands. The hypothalamus and pituitary gland in the brain regulate production through what is called the hypothalamic-pituitary-gonadal (HPG) axis.
Testosterone plays a critical role in many bodily functions beyond reproduction. It influences muscle mass and strength, bone density, red blood cell production, fat distribution, mood and motivation, cognitive function, and cardiovascular health. When levels drop below what your body needs, these systems can all be affected.
Production follows a daily rhythm - levels are highest in the morning and decline through the afternoon and evening. This is why diagnostic blood draws for testosterone are always performed in the morning.
What Are Normal Testosterone Ranges?
Most reference labs report total testosterone ranges of roughly 264 to 916 ng/dL for adult men. However, these ranges are based on population averages that include both healthy and unhealthy individuals. There are important nuances to understand.
Measures the total amount of testosterone in your blood, including both bound and unbound forms. The most common initial screening test.
The small percentage (typically 2-3%) that is not bound to proteins and is available for your body to use. Often a better indicator of how you feel day to day.
Sex hormone-binding globulin is a protein that binds testosterone and makes it unavailable. High SHBG can cause symptoms even when total testosterone looks normal.
Hormones from the pituitary gland that signal the testes to produce testosterone. These help determine whether low T is coming from the brain or the testes.
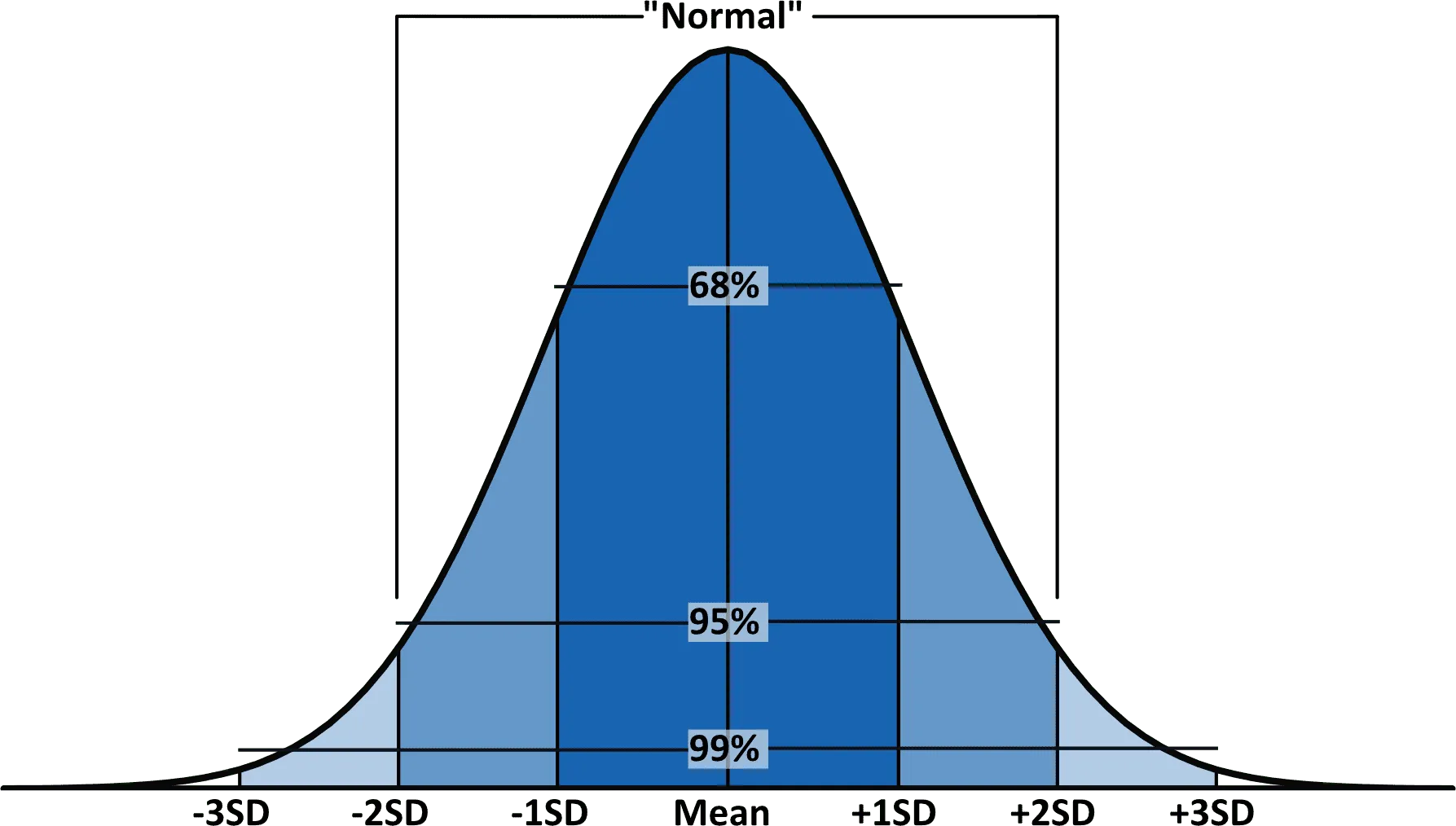
The Endocrine Society guidelines define hypogonadism (low testosterone) as a total testosterone consistently below 300 ng/dL on two or more morning blood draws. However, many men begin experiencing symptoms at levels well above that threshold, especially if their free testosterone is low or their SHBG is elevated. Symptoms and labs should be evaluated together - not in isolation.
What Is Low Testosterone (Low T)?
Low testosterone - sometimes called hypogonadism, low T, or testosterone deficiency - occurs when the body does not produce enough testosterone to maintain normal physiological function. It can be classified into two categories:
The testes themselves are not producing adequate testosterone. This can result from injury, infection (such as mumps orchitis), genetic conditions (like Klinefelter syndrome), or cancer treatments.
The pituitary gland or hypothalamus is not sending the right signals to the testes. This is more common and can result from obesity, insulin resistance, chronic stress, opioid use, sleep apnea, or aging.
Testosterone production naturally declines with age - roughly 1-2% per year after age 30. But age is only one factor. Lifestyle issues like poor sleep, chronic stress, sedentary behavior, excess body fat (especially visceral fat), and metabolic syndrome can accelerate the decline significantly. This is why some men in their 30s have testosterone levels lower than men in their 60s.
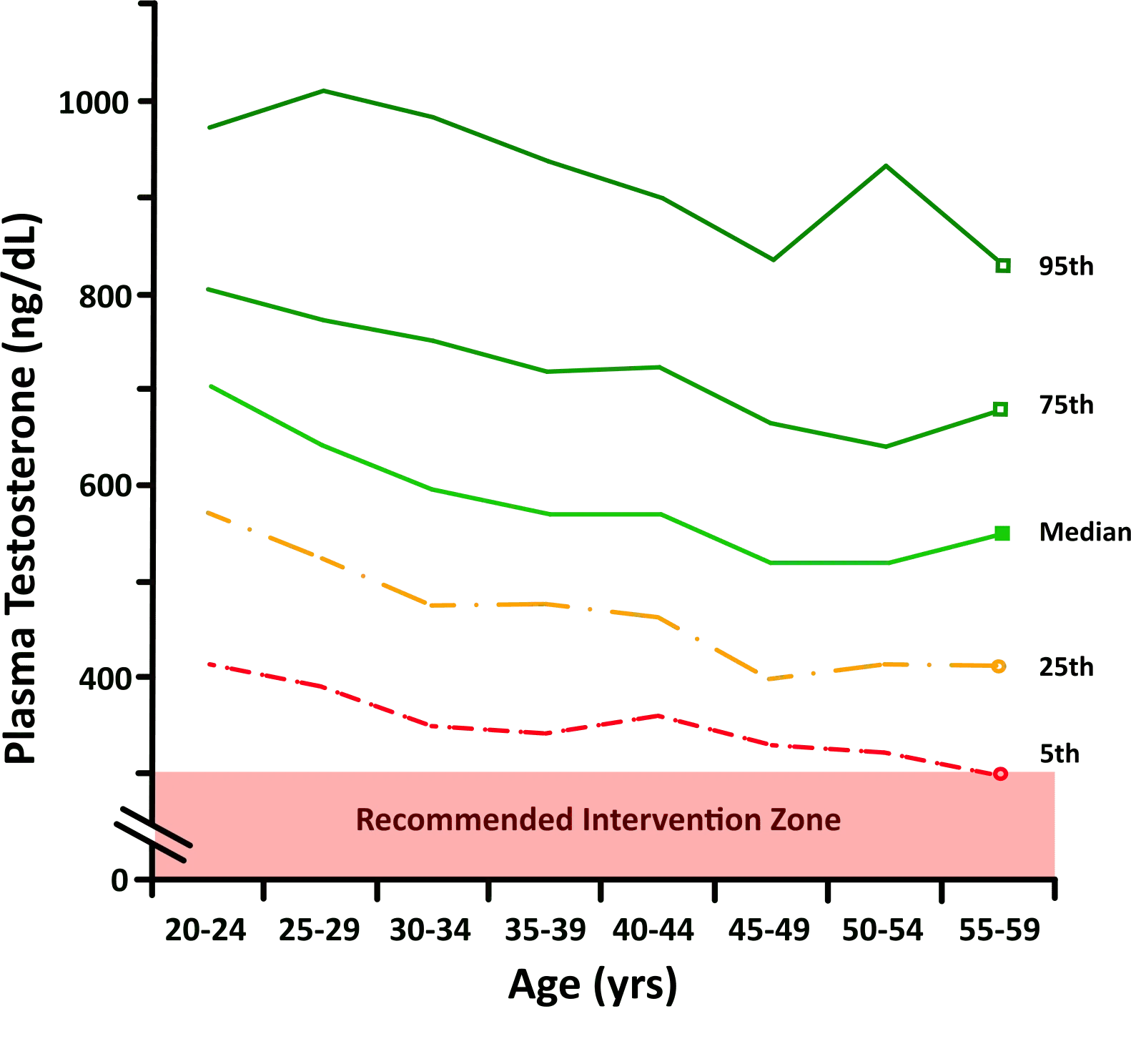
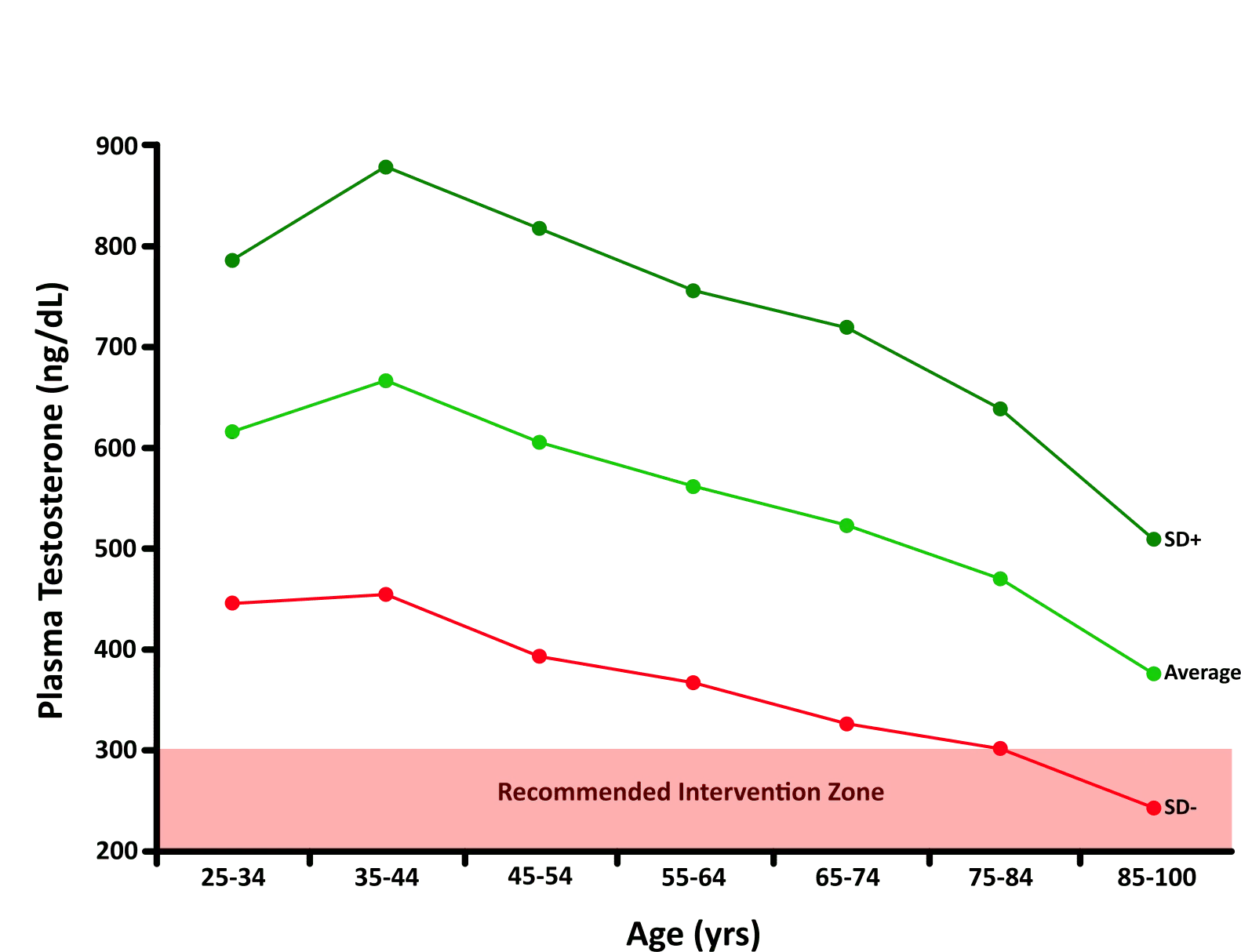
Symptoms of Low Testosterone
Low testosterone affects nearly every system in the body. Symptoms tend to develop gradually, which is why many men attribute them to "just getting older" rather than recognizing a treatable hormonal deficiency.
Not sure if your symptoms are related to testosterone? The Low Testosterone Quiz can help you assess whether an evaluation makes sense for your situation.
How Is Low Testosterone Diagnosed?
Proper diagnosis of low testosterone requires both symptoms and lab confirmation. Neither one alone is sufficient. A man can have a testosterone level of 280 ng/dL and feel perfectly fine, while another at 450 ng/dL may feel terrible depending on his free testosterone, SHBG, and other metabolic factors.
The Endocrine Society recommends confirming low testosterone with at least two morning blood draws showing total testosterone below 300 ng/dL, ideally drawn between 7:00 and 10:00 AM when levels are highest.
Symptom review and baseline blood draw
Full hormone and metabolic panel
Always included in a Focused Hormone Evaluation.
Added when the clinical picture warrants a deeper look. Available in the Complete Hormone or Total Wellness evaluations.
Why the layered approach? Low testosterone is often a downstream symptom of something else - insulin resistance, thyroid dysfunction, cortisol dysregulation, or elevated estrogen. The foundational panel confirms the diagnosis and identifies the most common drivers; additional studies are ordered when your symptoms or history point further upstream. A functional medicine approach looks at the full picture.
What Is Testosterone Replacement Therapy (TRT)?
Testosterone replacement therapy is a medical treatment that restores testosterone to physiologically normal levels in men whose bodies are not producing enough on their own. The goal is not to push testosterone to supraphysiological (bodybuilder) levels - it is to bring your levels back into a healthy, optimized range where symptoms resolve and your body functions the way it should.
TRT is prescribed and monitored by a licensed physician. It requires ongoing lab work to ensure levels stay within the target range and to monitor for any changes in hematocrit, estradiol, PSA, and metabolic markers. It is not the same as anabolic steroid use, which involves doses far beyond what the body naturally produces and carries significantly greater risk.
TRT Treatment Options
Several delivery methods exist for testosterone replacement. Each has its own advantages and considerations. The right choice depends on your lifestyle, preferences, and how your body responds.
The most common and cost-effective category. Testosterone cypionate is administered on a regular schedule - typically once or twice per week. Injections provide consistent, measurable levels and allow for precise dose adjustments. Two delivery routes are clinically equivalent options:
Injected into the muscle (deltoid or gluteal). The longest-studied route with decades of clinical data.
Injected into fatty tissue (abdomen or thigh) with a smaller needle. Equivalent absorption with potentially more stable levels.
Applied daily to the skin (shoulders, upper arms, or inner thighs). Testosterone absorbs through the skin and enters the bloodstream over several hours. This method avoids injections entirely but requires discipline with daily application and caution around skin-to-skin transfer to others.
Small pellets are implanted under the skin (usually in the hip or buttock area) during a quick in-office procedure. They slowly release testosterone over 3-6 months. This is a "set it and forget it" option for patients who prefer minimal ongoing maintenance.
At Asymmetric Health: we do not use pellet therapy except in a narrow group of male patients where injections and topicals are not viable, and we do not use pellets in women under any circumstances. Once implanted, dosing cannot be adjusted until the pellet is exhausted, which makes titration and side-effect management difficult.
Goals and Benefits of TRT
The goal of TRT is not simply to increase a number on a lab report. It is to restore quality of life by bringing testosterone back to a level where your body and mind function optimally. Research supports measurable benefits across multiple domains when low testosterone is properly treated.
Reduction in persistent fatigue, improved stamina and motivation throughout the day
Increased lean muscle mass, reduced visceral fat, and improved metabolic markers
Improved libido, erectile function, and overall sexual satisfaction
Clearer thinking, improved focus, better memory and mental processing speed
Reduced irritability, improved sense of well-being, decreased depressive symptoms
Increased bone mineral density, reducing the risk of fractures and osteoporosis
Improved lipid profiles, better insulin sensitivity, reduced inflammatory markers
More restorative sleep patterns and reduced nighttime waking
How Long Does It Take to Feel Results?
TRT is not an overnight fix. Different systems in the body respond on different timelines. The Testosterone Trials (TTrials), published in the New England Journal of Medicine in 2016, documented measurable improvements across all symptom domains within 12 months. Here is a general timeline based on clinical literature:
Energy, mood, motivation, sense of well-being
Libido and sexual interest, morning erections
Erectile function, fat loss begins, sleep improvement
Muscle mass gains, body composition changes, bone density
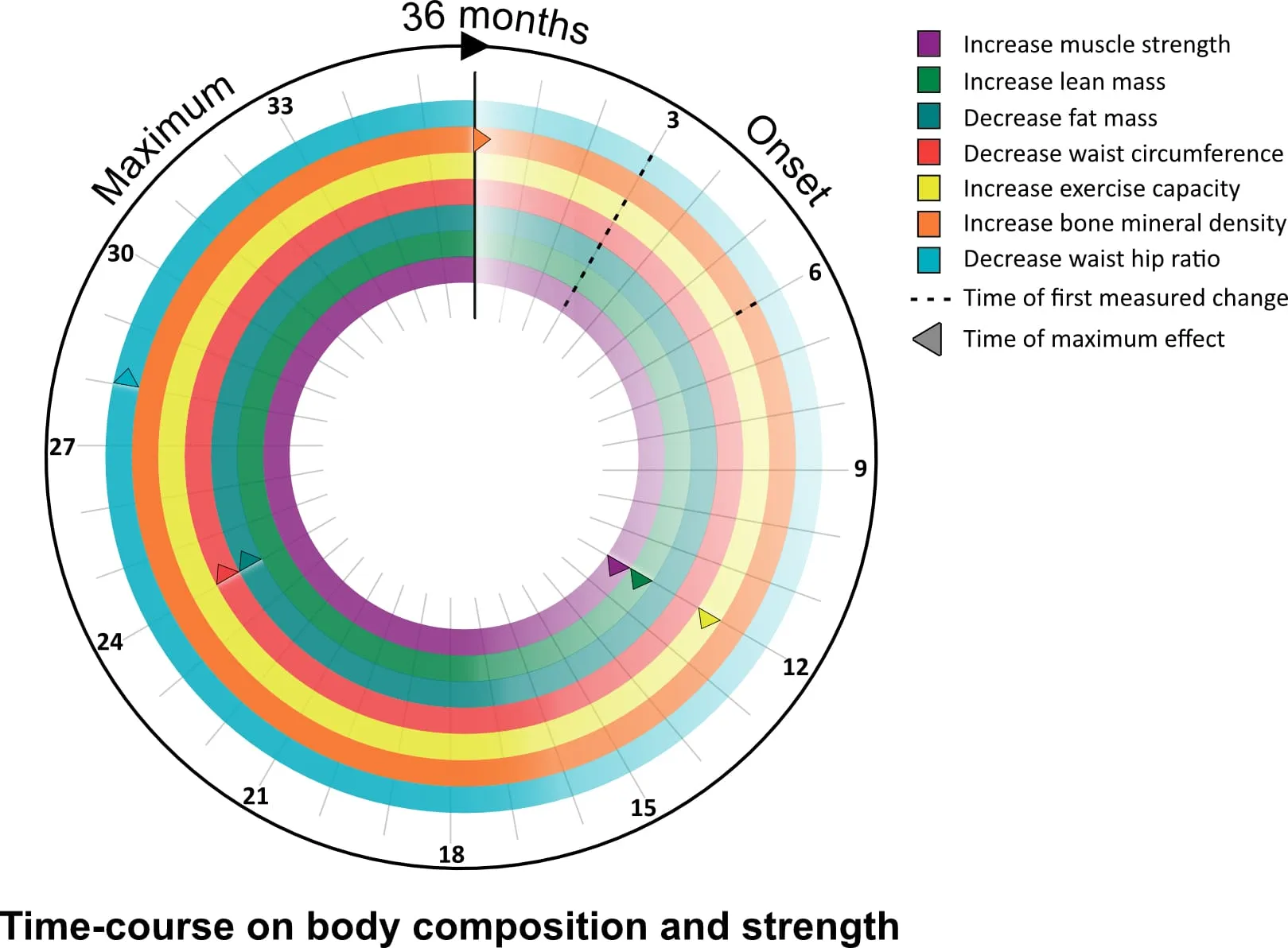
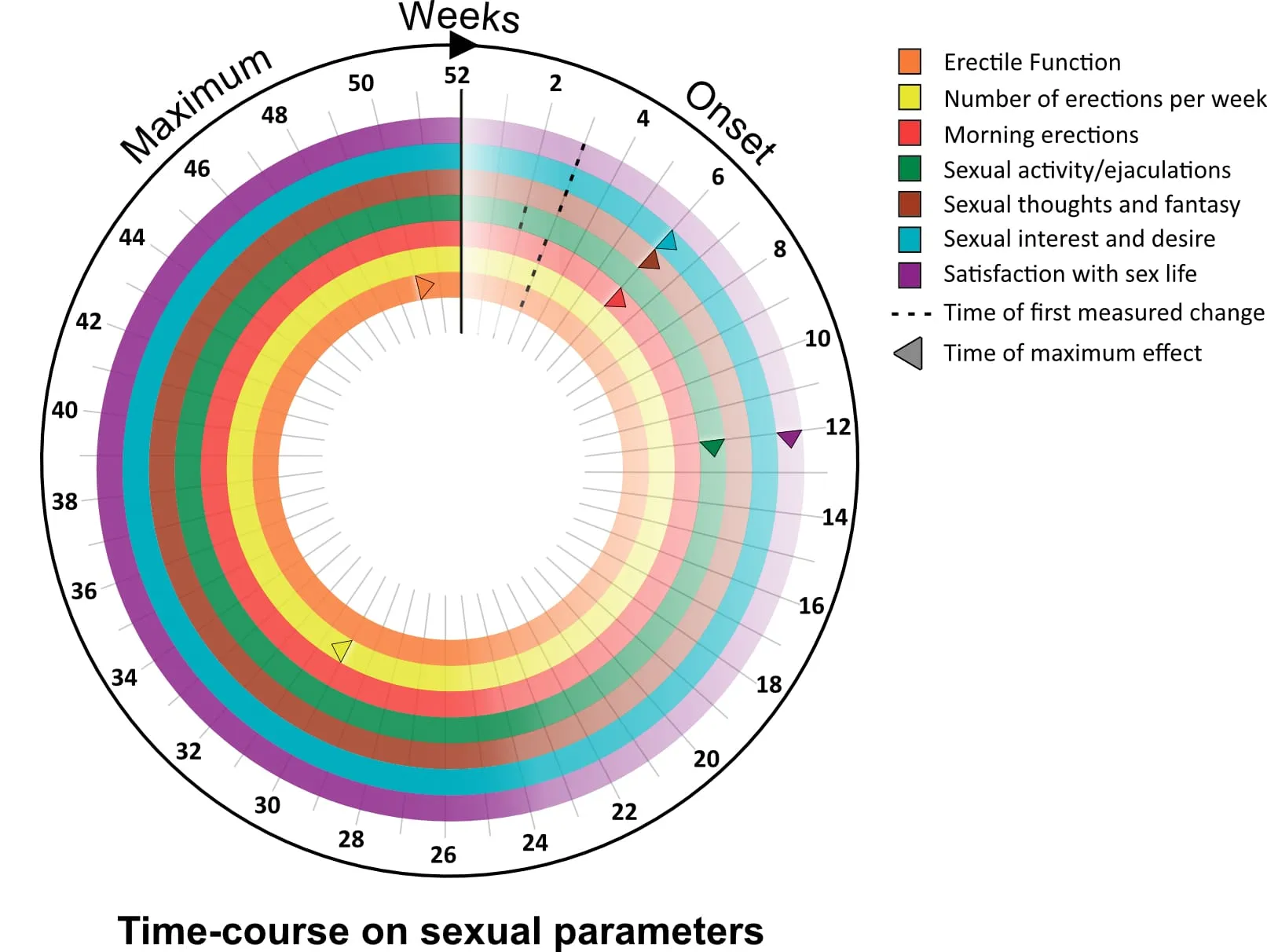
Individual timelines vary. Factors like starting testosterone level, overall health, body composition, sleep quality, and adherence to the protocol all influence how quickly you notice changes. Regular lab monitoring ensures your protocol is optimized over time.
Is TRT Safe?
This is one of the most common questions, and the research is encouraging. The TRAVERSE trial, published in the New England Journal of Medicine in 2023, was the largest randomized cardiovascular safety study of testosterone therapy ever conducted. It followed over 5,000 men aged 45-80 with hypogonadism and pre-existing cardiovascular risk factors for an average of 33 months.
The result: TRT did not increase the risk of major adverse cardiac events (heart attack, stroke, or cardiovascular death) compared to placebo. This was a landmark finding that addressed decades of concern about cardiovascular risk.
That said, TRT is a medical therapy that requires proper supervision. It is safe when prescribed by a knowledgeable physician, dosed appropriately, and monitored regularly with lab work. The risks come from unsupervised use, excessive dosing, or failure to monitor key markers like hematocrit and estradiol.
Potential Side Effects of TRT
Like any medical therapy, TRT carries potential side effects. Most are manageable with proper monitoring and dose adjustments. Awareness and regular lab work are the best prevention.
TRT stimulates red blood cell production. If hematocrit rises too high, blood becomes thicker, which can increase clotting risk. Regular CBC monitoring catches this early. Dose adjustment, hydration, or therapeutic phlebotomy (blood donation) can manage it.
Testosterone can convert to estradiol via the aromatase enzyme, especially in men with higher body fat. Elevated estrogen can cause water retention, mood changes, or gynecomastia (breast tissue growth). Monitoring estradiol levels and adjusting protocol accordingly prevents this.
Exogenous testosterone suppresses the body's own production via negative feedback on the HPG axis. Over time, this can cause the testes to shrink. HCG (human chorionic gonadotropin) can be included in the protocol to maintain testicular function.
TRT suppresses sperm production (spermatogenesis). For men who want to maintain or preserve fertility, HCG or other fertility-preserving strategies should be part of the treatment plan. This is an important discussion to have before starting therapy.
Some men experience increased oiliness or acne, particularly in the first few months. This typically stabilizes as the body adjusts to new hormone levels.
TRT may worsen pre-existing sleep apnea in some patients. If you snore heavily or have untreated sleep apnea, this should be evaluated before starting therapy.
The key takeaway: side effects are real but manageable. The difference between a good outcome and a problematic one comes down to the quality of monitoring. Regular lab work and an attentive provider who adjusts your protocol based on your response - not a one-size-fits-all approach - make TRT both effective and safe.
Ready to Find Out Where You Stand?
If you are experiencing symptoms of low testosterone, the first step is a proper hormone evaluation. At Asymmetric Health, the Focused Hormone Evaluation covers the male hormone axis (12+ markers including total/free testosterone, estradiol, SHBG, LH/FSH, PSA, hematocrit, and supporting metabolic markers), a 60 minute consultation with your provider, and a personalized treatment plan.
Not sure yet? Take the Low Testosterone Quiz to see if an evaluation makes sense for you.
